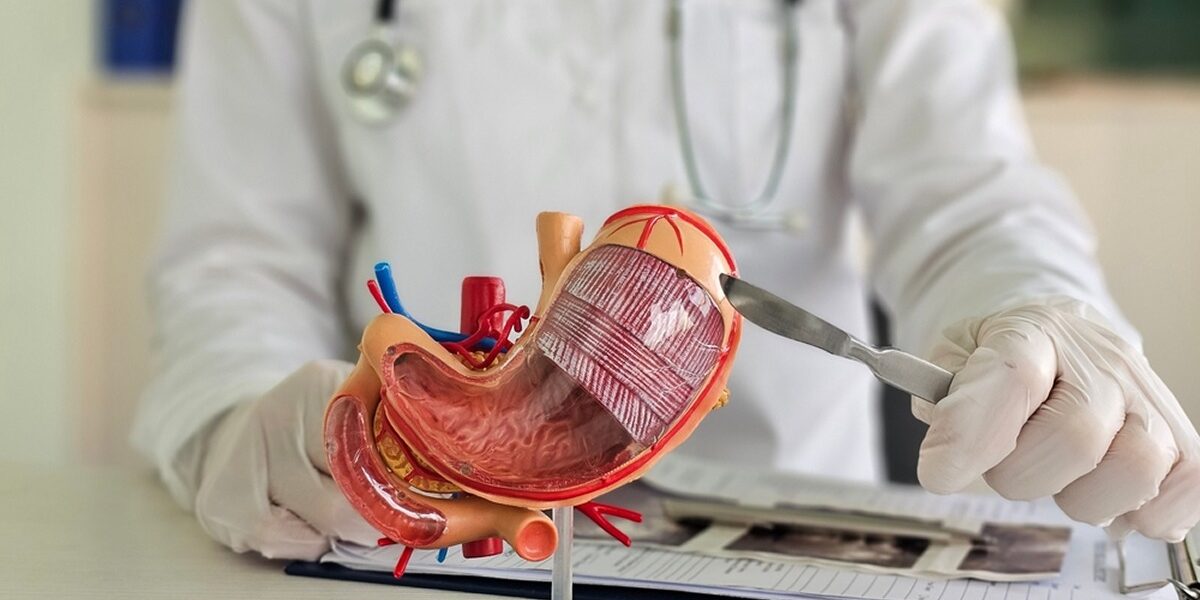
Bariatric surgery is one of the most effective long-term interventions for severe obesity and obesity-related health conditions. Whether you are exploring it as a patient, researching as a healthcare professional, or studying outcomes as a weight loss researcher, understanding what bariatric surgery means, how it works, and what to expect is essential to making informed decisions.
In this comprehensive guide, we cover the definition and types of bariatric surgery, what the surgical process looks like, expected results, potential complications, and the average cost involved, answering the most common questions patients and clinicians ask.
1. Understanding Bariatric Surgery
Bariatric Surgery Definition and Overview
The bariatric surgery meaning comes from the Greek word “baros” (weight) and “iatros” (physician). Medically defined, bariatric surgery refers to a group of surgical procedures that modify the gastrointestinal tract to help individuals with severe obesity lose weight. These procedures either restrict the amount of food the stomach can hold, reduce nutrient absorption, or a combination of both.
According to the American Society for Metabolic and Bariatric Surgery (ASMBS), more than 200,000 bariatric surgeries are performed annually in the United States, making it one of the most commonly performed abdominal procedures in the country.
📋 Key Definition
Bariatric surgery is a collective term for weight-loss surgeries that alter the digestive system to help patients with obesity achieve sustained weight loss and improve related health conditions.
Importance of Bariatric Surgery for Obesity
Obesity is categorized as a complicated, long-term illness. When lifestyle interventions such as diet, exercise, and medications fail to produce adequate results, bariatric surgery becomes a medically recommended option. It is typically considered for individuals with:
- A Body Mass Index (BMI) of 40 or higher (Class III obesity)
- A BMI of 35–39.9 with at least one serious obesity-related condition such as type 2 diabetes, hypertension, or sleep apnea
- A BMI of 30–34.9 with uncontrolled type 2 diabetes or metabolic syndrome in select cases
Bariatric surgery not only facilitates significant weight loss but also leads to remission or improvement of multiple comorbidities, dramatically enhancing quality of life.
How Bariatric Surgery Works in the Body
Bariatric surgery works through three primary mechanisms:
- Reducing stomach size limits the quantity of food that can be consumed at one time.: Restriction
- Bypassing parts of the small intestine reduces the calories and nutrients the body absorbs.: Malabsorption
- Surgery can alter hunger-regulating hormones like ghrelin, reducing appetite and improving metabolic function.: Hormonal changes
These combined mechanisms create a sustained caloric deficit and metabolic shift that supports long-term weight management, something that cannot be replicated by diet or medication alone.
2. Types of Bariatric Surgery
Understanding the different types of bariatric surgery is critical for both patients and clinicians. Each type carries unique benefits, risks, and eligibility criteria. Below is an overview of the most common bariatric surgery types.
Gastric Bypass Surgery (Roux-en-Y Gastric Bypass)
Gastric bypass surgery is widely considered the gold standard of bariatric procedures. It involves two steps:
- A small pouch (about the size of an egg) is created at the top of the stomach, drastically limiting food intake.
- The small intestine is rerouted so that food bypasses the majority of the stomach and the upper small intestine, reducing calorie and nutrient absorption.
Gastric bypass typically results in 60–80% excess weight loss within 12–18 months and has a strong track record for resolving type 2 diabetes, sometimes even before significant weight loss occurs.
📋 Best For
Patients with severe obesity (BMI ≥ 40), type 2 diabetes, or severe acid reflux who are seeking maximum weight loss results.
Sleeve Gastrectomy (Gastric Sleeve)
Sleeve gastrectomy, commonly called a “gastric sleeve,” involves removing approximately 75–80% of the stomach, leaving a narrow, banana-shaped sleeve. This procedure:
- Significantly restricts food intake
- Reduces the production of ghrelin, the hunger hormone
- Does not reroute the intestines, making it a simpler procedure with fewer long-term nutrient deficiency risks
It is currently the most commonly performed bariatric procedure in the U.S., accounting for roughly 60% of all weight-loss surgeries.
📋 Best For
Patients looking for effective weight loss with a lower surgical complexity, or those who are not good candidates for intestinal bypass.
Other Types of Bariatric Surgery
Adjustable Gastric Band (Lap-Band)
An inflatable silicone band is placed around the upper portion of the stomach to create a small pouch. Over time, the band can be changed. While less invasive, it has largely fallen out of favor due to lower efficacy and higher rates of long-term complications.
Biliopancreatic Diversion with Duodenal Switch (BPD/DS)
This is one of the most complex bariatric procedures, combining a sleeve gastrectomy with a significant intestinal bypass. It produces the greatest weight loss of any bariatric surgery but also carries the highest risk of nutritional deficiencies, and is reserved for patients with extreme obesity (BMI ≥ 50).
Single Anastomosis Duodeno – ileal Bypass with Sleeve (SADI-S)
A newer, simplified version of the BPD/DS that offers strong weight loss results with fewer complications. It is gaining acceptance and is now performed at specialized bariatric centers.
3. Bariatric Surgery Process
Pre-Surgery Evaluations and Requirements
Before any bariatric procedure, patients undergo a comprehensive multi-disciplinary evaluation. The bariatric surgery process begins well before the operating room:
- Medical evaluation including bloodwork, cardiac testing, and metabolic assessment
- Nutritional counseling and a pre-operative diet (often a 2–4 week low-calorie or liquid diet)
- Psychological evaluation to assess readiness and identify any behavioral health concerns
- Documented attempts at non-surgical weight loss (diet, exercise, medications)
- Clearance from a bariatric surgeon and, in some cases, an endocrinologist or cardiologist
Insurance providers typically require a minimum of 3–6 months of documented physician-supervised weight loss efforts before approving coverage for surgery.
Step-by-Step Surgical Procedure
Most bariatric surgeries today are performed laparoscopically, meaning through small incisions using a camera (laparoscope) and specialized instruments. This minimally invasive approach reduces recovery time and lowers complication risk.
A typical laparoscopic bariatric procedure follows these steps:
- General anesthesia is administered
- The surgeon makes 3–5 small incisions in the abdomen
- A laparoscope and surgical tools are inserted through the incisions
- The chosen procedure (bypass, sleeve, etc.) is performed
- Incisions are closed; the patient is moved to recovery
Most procedures take between 1–3 hours depending on complexity and the type of bariatric surgery performed.
Post-Operative Care and Recovery
Recovery from bariatric surgery typically involves a hospital stay of 1–3 days. Long-term success depends on post-operative care.
- Diet progression from clear liquids to solid foods over 6–8 weeks
- Daily vitamin and mineral supplementation (iron, calcium, B12, vitamin D)
- Regular follow-up visits at 1 month, 3 months, 6 months, and annually
- Physical activity increases gradually starting 4–6 weeks post-surgery
- Ongoing nutritional counseling and behavioral support
📋 Important
Adherence to post-operative dietary guidelines and vitamin supplementation is essential to prevent nutritional deficiencies and maximize weight loss outcomes.
4. Bariatric Surgery Results
Expected Weight Loss Outcomes
One of the most frequent queries from patients is: What are the realistic outcomes of bariatric surgery? The answer varies depending on the type of procedure, initial weight, and compliance with post-surgical protocols.
.General expected outcomes by procedure:
- Gastric Bypass: 60–80% excess weight loss within 12–18 months
- Sleeve Gastrectomy: 50–70% excess weight loss within 18–24 months
- Adjustable Gastric Band: 40–50% excess weight loss over 2–3 years
- BPD/DS: 70–80%+ excess weight loss, the highest of any procedure
Within 12 to 24 months following surgery, the majority of patients achieve their maximum weight loss. Research shows that the majority of patients maintain 50% or more of their excess weight loss at the 5-year mark when behavioral guidelines are followed.
Improvements in Health Conditions
Beyond weight loss, bariatric surgery produces remarkable improvements in obesity-related comorbidities:
- Type 2 Diabetes: Remission in up to 80% of patients after gastric bypass
- Hypertension: Resolved or improved in over 75% of patients
- Obstructive Sleep Apnea: Resolved in approximately 85% of cases
- High Cholesterol: Normalized in over 70% of patients
- Joint Pain and Osteoarthritis: Significant reduction with weight loss
- GERD (Acid Reflux): Improved with sleeve gastrectomy; may worsen with some procedures, discuss with your surgeon
Long-Term Success and Maintenance
Surgery alone does not guarantee long-term success after bariatric surgery.. Sustained results depend on:
- Commitment to lifelong dietary changes and portion control
- Regular physical activity
- Ongoing follow-up with the bariatric care team
- Psychological support and behavior services when needed
- Vitamin and supplement compliance for life
Studies show that patients who engage with long-term support programs have significantly better weight maintenance outcomes than those who do not continue follow-up care.
5. Bariatric Surgery Complications and Costs
Potential Complications of Bariatric Surgery
Bariatric surgery, like any other major surgery, has risks. Understanding potential bariatric surgery complications allows patients to make fully informed decisions.
Short-Term Complications
- Bleeding, infection, or blood clots (deep vein thrombosis)
- Anastomotic leaks (in gastric bypass), a serious but rare complication
- Adverse reactions to anesthesia
- Pulmonary embolism
Long-Term Complications
- Nutritional deficiencies (vitamin B12, iron, calcium, vitamin D)
- Dumping syndrome, rapid gastric emptying causing nausea, diarrhea, and lightheadedness after eating sugar or high-fat foods
- GERD and acid reflux (more common with sleeve gastrectomy)
- Weight regain, especially without behavioral support
- Gallstones (risk increases with rapid weight loss)
- Band slippage or erosion (specific to adjustable gastric band)
Overall, the 30-day mortality rate for bariatric surgery is approximately 0.1–0.3%, comparable to a laparoscopic gallbladder removal, making it one of the safer major surgeries performed today.
Frequently Asked Questions About Bariatric Surgery
What is bariatric surgery and how does it work?
Bariatric surgery is a group of weight-loss procedures that modify the stomach and/or small intestine to limit food intake, reduce nutrient absorption, or alter hunger hormones. It is recommended for individuals with severe obesity when non-surgical methods have not produced adequate results.
What are the different types of bariatric surgery?
The main types of bariatric surgery include gastric bypass (Roux-en-Y), sleeve gastrectomy, adjustable gastric band, and biliopancreatic diversion with duodenal switch (BPD/DS). The most commonly performed procedures today are the gastric sleeve and gastric bypass.
What complications can arise from bariatric surgery?
Complications can be short-term (bleeding, infection, anastomotic leak) or long-term (nutritional deficiencies, dumping syndrome, acid reflux, weight regain). Thorough pre-operative evaluation and post-operative follow-up significantly reduce these risks.
What results can patients expect after bariatric surgery?
Most patients can expect 50–80% excess weight loss depending on the procedure, along with significant improvement or resolution of type 2 diabetes, hypertension, sleep apnea, and other obesity-related conditions. Long-term success depends on dietary adherence and ongoing care.
How much does bariatric surgery usually cost?
In the United States, bariatric surgery costs range from $10,000 to $45,000 depending on the procedure. Many insurance plans cover surgery if medical necessity criteria are met. International options can significantly reduce out-of-pocket costs.
Conclusion
Bariatric surgery represents a life-changing option for individuals living with severe obesity. By understanding the bariatric surgery definition, the various types of bariatric surgery, the surgical process, expected results, potential complications, and financial considerations, patients and healthcare teams can make well-informed, collaborative decisions.
If you or a patient is considering bariatric surgery, consulting with a board certified bariatric surgeon and a multidisciplinary weight management team is the essential first step toward a healthier future.